Heidelberg 30 June 2025. We recently studied cases of IOL exchange and in April this year published our results in Scientific Reports, the peer-reviewed open-access journal published by Nature Portfolio:
Henningsen N, Khoramnia R, Auffarth GU, Köppe MK, Łabuz G, Yildirim TM. Visual and refractive outcome, higher order aberrations and complications following intraocular lens exchange in eyes without comorbidities. Sci Rep. 2025 Apr 23;15(1):14202. doi: 10.1038/s41598-025-98931-y. PMID: 40269218; PMCID: PMC12019354.
Background
In cases with severe IOL-related complications, IOL exchange is often the best treatment option. There is limited published data on the impact of this procedure on refractive outcomes and intra- and postoperative complications, particularly in patients with otherwise healthy eyes.
What did we do?
We investigated the refractive outcome of IOL exchange surgery, including corneal aberrations, and assessed the influence of different IOL characteristics on intraoperative and postoperative complications.
Our methods
We conducted a prospective clinical study that included 35 eyes with homogeneous IOL calcification and no other ocular pathologies. We measured the eyes’ corrected distance visual acuity (CDVA) using the Pentacam AXL Wave (Oculus Optikgeräte GmbH, Wetzlar, Germany), comparing target refraction to the postoperative spherical equivalent. Corneal topography and lower- and higher-order aberrations were assessed preoperatively and 3 months postoperatively.
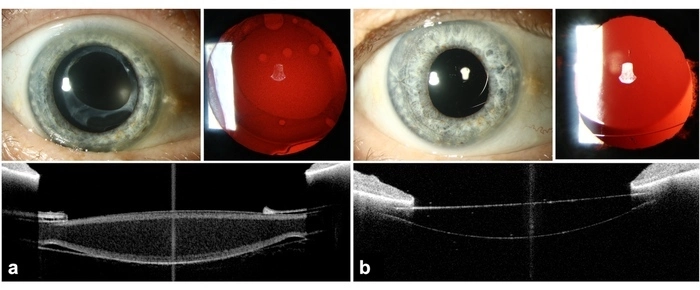
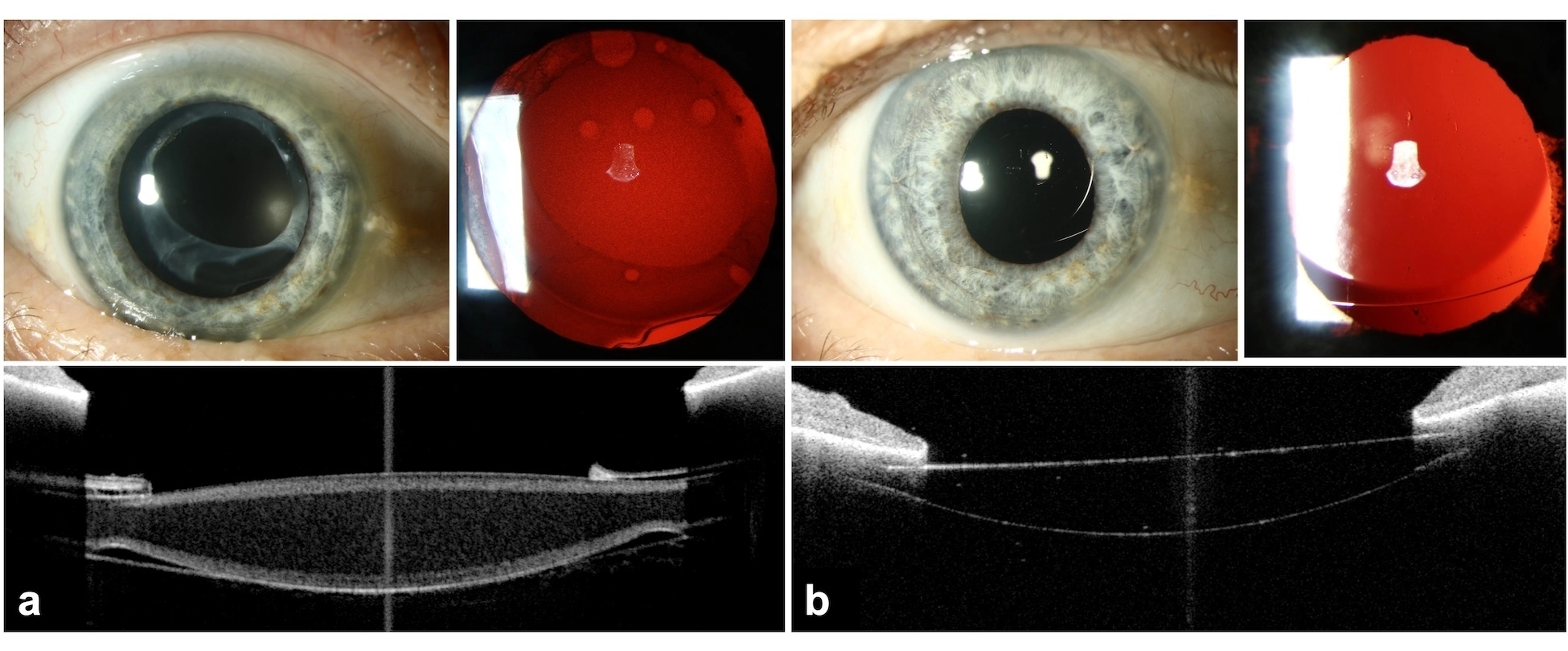
- Photo montages of a. before IOL exchange and b after IOL exchange
We also recorded intraoperative and postoperative complications and compared these complications between different IOL characteristics.
Our results
The secondary IOL in 53% of cases, was a retropupillary iris-fixated Artisan Aphakia (Ophtec BV, Groningen, Netherlands), 37% had a sulcus-fixated AR40e (Johnson & Johnson Vision, Irvine, USA), and 10% received a capsular bag IOL. The CDVA improved from 0.16 ± 0.14 to 0.07 ± 0.14 logMAR (p = 0.04). In most cases, the target refraction was within ± 1.0 D (Artisan: 71%, AR40e: 90%, Capsular: 100%). IOL exchange did not induce relevant change in corneal aberrations. Anterior (81%) and posterior (78%) vitrectomy were performed in most cases.
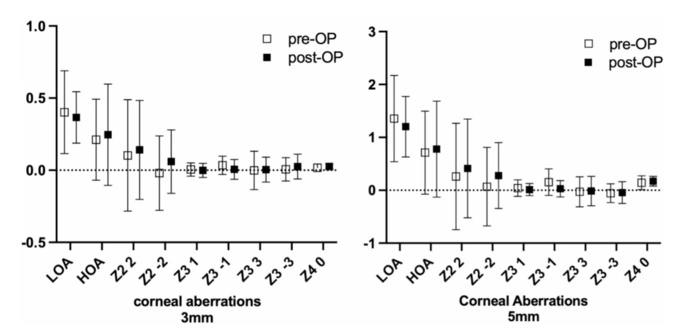
- Corneal aberrations at 3mm and 5mm The graphs show Corneal lower and higher order aberrations (LOA/ HOA), horizontal and vertical astigmatism (Z2 2, Z2 -2), coma (Z3 1, Z3 -1), trefoil (Z3 3, Z3 -3) and spherical aberrations (Z4 0) pre- and post-operative for the 3 mm and 5 mm zone. Mean values in Diopter (D) with standard deviation.
We noted that the haptic design of the primary IOL did not affect intra- or postoperative complications.
Our Conclusions
Although exchanging an IOL involves greater surgery compared to the initial IOL implantation, visual and refractive outcomes are generally good, and the exchange does not cause a significant change in aberrations. Intra- and postoperative complications are mostly mild and resolve without sequelae.
Our paper is open access, and the link to view it is:


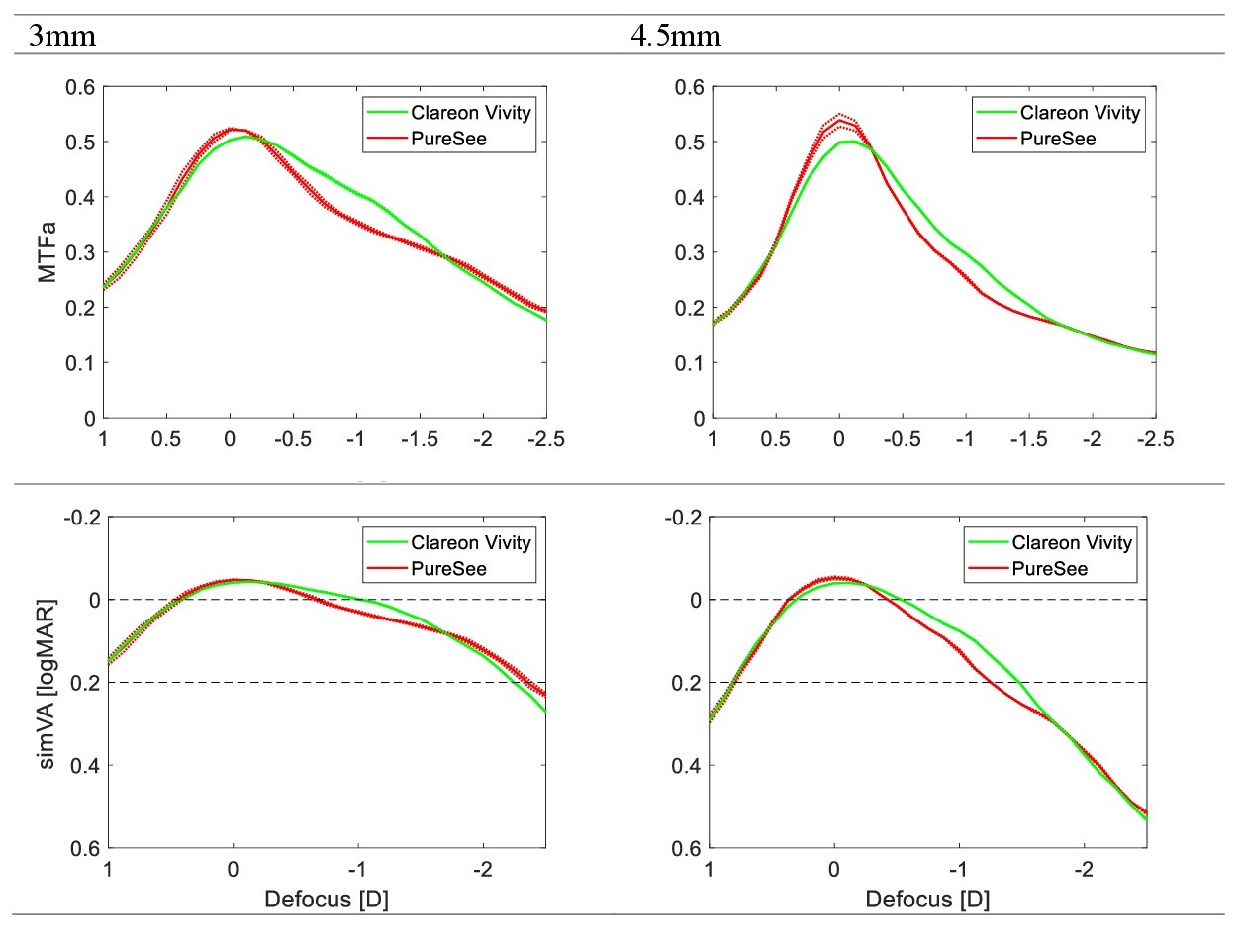
 Simulating IOL vision before implanting a lens
Simulating IOL vision before implanting a lens