I’m very glad that a case report on IOL calcification we made with colleagues at St Thomas’s Hospital in London has finally been published in the American Journal of Ophthalmology Case Reports, a companion title to the prestigious American Journal of Ophthalmology.
Intraocular lens calcification in a patient with Ehlers-Danlos syndrome
Matthew J. Maguire,Donald John Munro,Patrick Merz,Alistair Laidlaw,Gerd U. Auffarth Publication: American Journal of Ophthalmology Case Reports Publisher: Elsevier
IOL Calcification
We emphasise that Calcification is a rare complication following cataract surgery. In some cases, the problem was traced to the IOL manufacturer and that can be termed Primary Calcification. But there are also cases of what we call Secondary Calcification. The lens is manufactured correctly, but something in the implantation operation or intrinsic to the patient acts as a potentiator for Calcification. This Secondary Calcification is due to patient host factors, changes in the IOL’s micro-environment in the eye, or is provoked by the patient’s condition - uveitis, proliferative diabetic retinopathy or the sequelae of ocular surgery.
What was different this time?
Until we encountered this rare case, systemic connective tissue disease had not been linked to IOL opacification. Our colleagues in St Thomas’s describe the clinical presentation and management of a young patient with a rare subtype of Ehlers-Danlos syndrome. The patient presented with secondary IOL calcification 14 years after the IOL had been implanted. The IOL was explanted and sent to our laboratory.
What could we find?
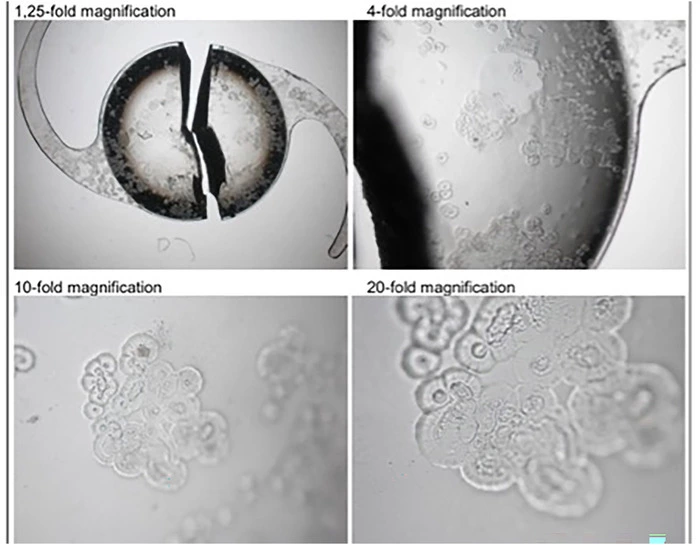
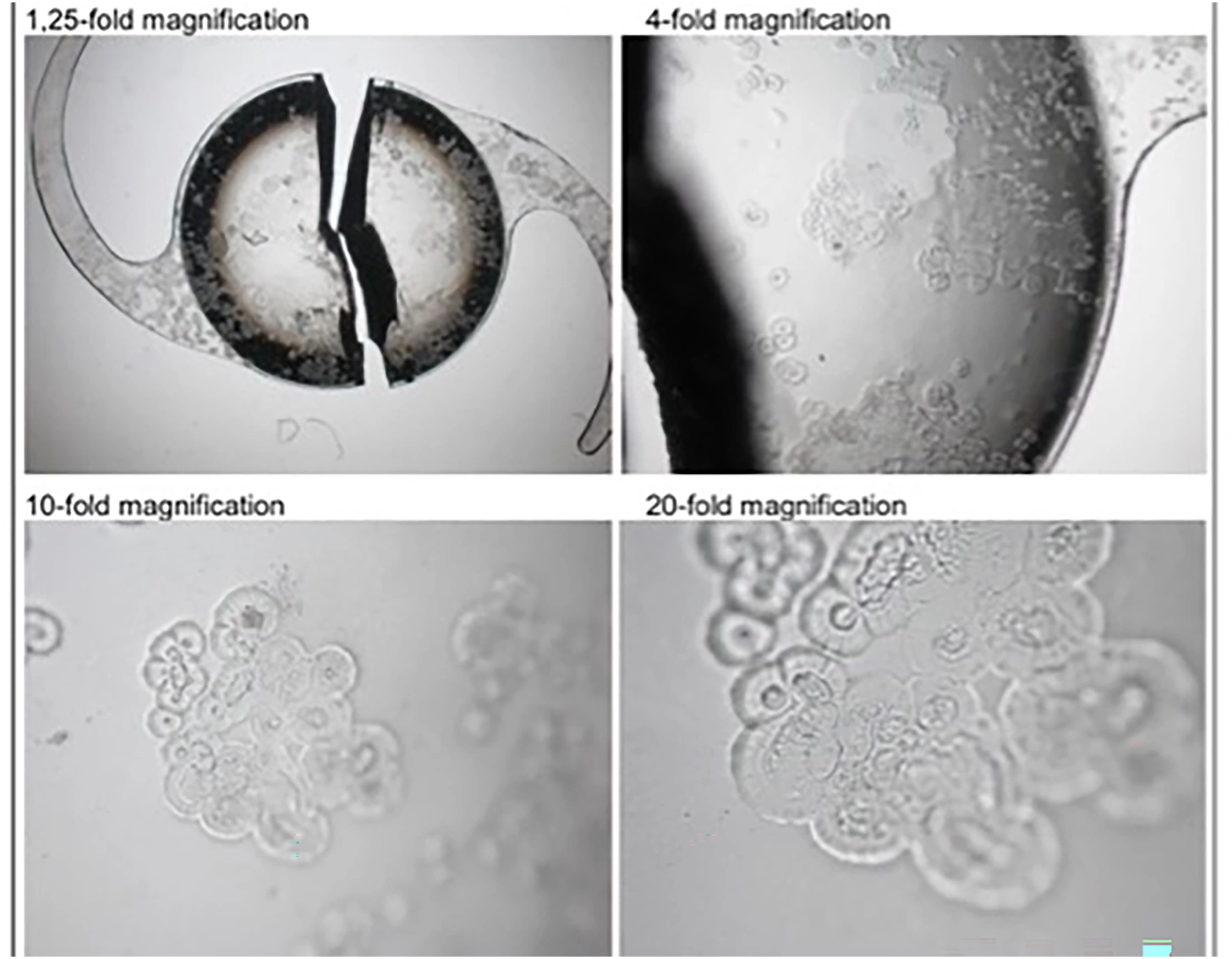
In our laboratory, we observed Floret-like lesions on the IOL surface.
We found positive histopathological staining for Calcification with the Alizarin red;
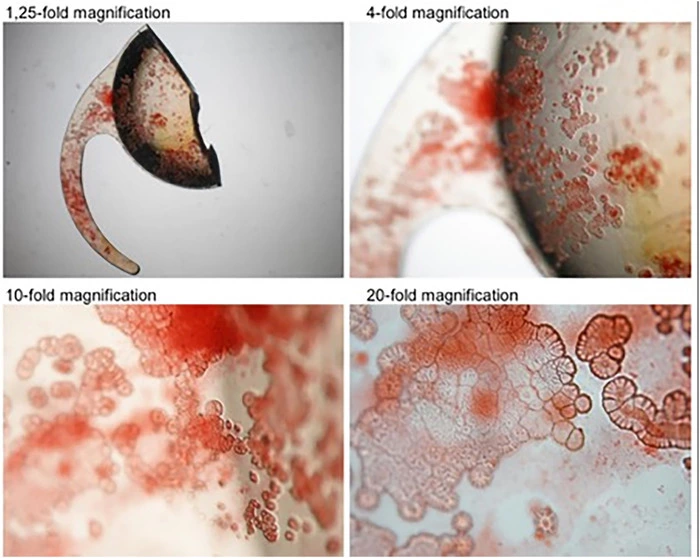
and with the von Kossa method we demonstrated calcium phosphate deposits beneath the whole IOL surface.
Our Conclusions
Patients with systemic connective tissue disease, such as a subtype of Ehlers-Danlos, may present with secondary IOL calcification many years after the lens has been implanted. Surgeons should consider carefully the choice of IOL when planning cataract surgery in these patients. In this case, good visual acuity was achieved when the surgeons exchanged the IOL for a new model.
Our paper will appear in print in September 2024 but is now available online in open access, using the publisher’s link to the article.
The David J Apple Laboratory continues to accept explant lenses from surgeons worldwide. Here is the link to the form for reporting IOL explantation.


 New IOL material - xPIB
New IOL material - xPIB